AR Analysis And Recovery
Turning Accounts Receivable Into Actual Revenue

Accelerate Your AR Recovery By Leveraging Our Expert Accounts-Receivable Analysis
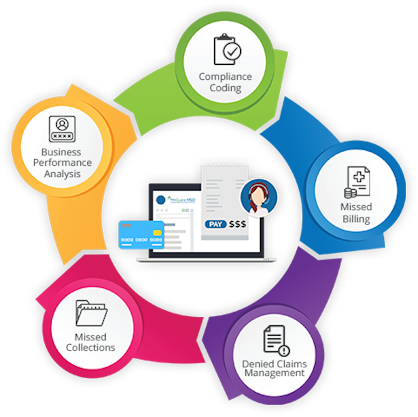
Compliance Coding
The process begings with accurate documentation and translation of medical services into standardized codes (ICD-10, CPT, etc) to ensure compliance with payer rules and reduce inital claim rejections.
Preventing Missed Billing
Rigorous checks are put in place to ensure all bilable services are captured and documented correctly, preventing revenue leakage from services rendered but not invoiced.
Denied Claims Management
Unpaid or rejected claims are tracked and analyzed to identify the root cause of denials. This crucial step involves correcting errors, gathering necessary information, and appealing the denials in a timely manner to recover lost revenue.
Reducing Missed Collections
This involves persistent follow-up on outstanding balances, both from insurance companies and patients. Clear communication and flexible payment options help ensure timely payment and reduce the likelihood of accounts being written off as bad debt.
Business Performance Analysis
The entire cycle is continuously monitored using key performance indicators (KPIs) like denial rates and days in AR. This data driven analysis helps management identify trends, find bottlenecks, and optimize the overall billing and collection processes.
Payment Processing
The goal of the cycle is the receipt and application of payments from insurance comapnies and patients. Once received, payments are accurately posted to the current accounts and reconciled with the initial invoices.
Why Choose Us?

Reduce Loss
Our robust Accounts Receivable (AR) analysis identifies denied, underpaid, and aging claims before they become write-offs. By proactively correcting errors, submitting timely appeals, and pursuing underpayments, we recover revenue that might otherwise be lost and protect your practice from unnecessary financial leakage.
Data Driven Decision Making
Comprehensive analysis of AR reports allows us to identify patterns in claim denials, payer performance, reimbursement trends, and patient payment behavior. By turning data into actionable insights, we help practices make informed operational and financial decisions that improve collections, reduce risk, and strengthen long-term profitability.

Improved Cash Flow
Timely collection of payments from both insurers and patients ensures consistent and predictable cash flow—critical for meeting payroll, covering operational expenses, and supporting continued growth. Our proactive follow-up and structured processes reduce payment delays and keep your revenue moving efficiently..
More Info

Affiliations

Affiliations

